Previous ulceration is defined as an area that has previously been ulcerated but has subsequently healed. After ulceration the affected area never repairs itself completely and only returns to 70% of tensile strength. This area is always vulnerable to future ulcerations. Previous ulceration is the highest risk factor for future ulceration.
Category: The procedure (NHS Scotland)
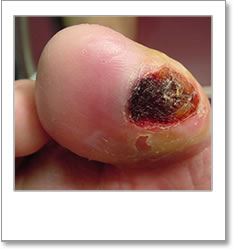
Active ulceration (6/17)
Active ulceration (pictures below) is defined by The International Working Group on the Diabetic Foot 2005 (IWGDF), as:
‘a full thickness wound, i.e. a wound penetrating through the dermis, below the ankle in a diabetic patient, irrespective of duration’.
In Scotland the TEXAS scale is generally used to classify a diabetic foot ulcer: Texas Scale [.pdf, 1.72 MB].
If during the screening process you discover the individual has a foot ulcer the individual should be referred without delay for treatment/management by an experienced podiatrist who is part of a multidisciplinary foot team/service.

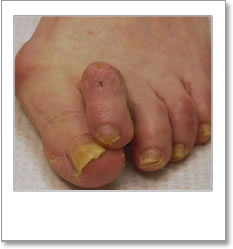
Structural abnormality of the foot (5/17)
Structural abnormality of the foot (pictures below) is defined as:
‘A change in foot shape that resulted in a difficulty in fitting shoes which could be purchased in high street shops’. (Scottish Diabetes Group – Foot Action Group 2010).


A non significant structural abnormality of the foot can be described as a very minor change of shape of the foot which does not result in areas of pressure, leading to callus formation, and a difficulty in fitting shoes which could be purchased in high street shops.
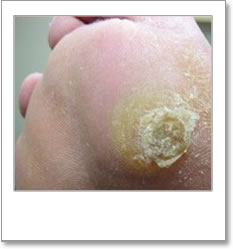
Significant callus (4/17)
Significant callus (pictures below) is defined as:
‘Callus that requires Podiatric Management’ (Scottish Diabetes Group – Foot Action Group 2010).
Significant callus causes pressure on the underlying tissues which can result in the tissues breaking down and an ulcer developing. If an individual has significant callus and is not attending a podiatrist then they should be referred to have a treatment/management plan agreed and introduced to suit their needs.


Non significant callus can be described as callus that does not require podiatric treatment, does not pose any risk and can be treated/managed by the individual.
The treatment of non significant callus or areas of dry skin can be managed by the individual after some simple instruction. The careful use of emery boards/ pumas stone, the regular application of a moisturiser cream and by following the advice given in the Low risk leaflet will usually achieve this.
Starting the screening process (3/17)
To start the screening process you should:
- Seat individual on examination couch/chair
- Inform the individual that you are going to examine their feet to check their circulation, sensation and any other risk factors that they might have which could lead to a foot problem related to their diabetes
- Request individual remove shoes and socks/stockings and assist if required
Ascertain if…
- The individual is experiencing any problems with their feet
- Has the individual noticed any changes since their last visit?
- If complaining of podiatric type problems (corns, nail problems etc.) check if currently attending a Podiatrist and refer/treat if necessary.
Recording of foot screening information (2/17)
The SIGN 116 guidelines recommend that foot screening information is recorded electronically which can be shared between all health care professionals, as stated in the Sign 116 Guideline:
‘The result of a foot screening examination should be entered onto an online screening tool, such as the Scottish Care Information – Diabetes Collaboration system (SCI-DC),(now known as SCI – Diabetes) to provide automatic risk stratification and a recommended management plan, including patient information‘.
SCI-Diabetes is being established as the national IT system for Diabetes to support individuals and diabetes managed clinical networks across NHS Scotland.

There are many advantages of using the SCI-Diabetes foot screening tool:
- To prevent duplication of effort (at present some screening data recording is carried out on systems that do not share the information with all the Health Care Professionals involved in the individuals care or is ‘paper based’ and is not easily shared)
- Any suitably trained HCP who sees the individual can carry out the foot screening using the SCI-Diabetes system
- Using SCI-Diabetes the information is recorded and stored centrally so it can be accessed by all HCP´s involved in the individual´s care who will be able to see when the last screening was carried out and what the individuals risk status was.
- When the screening information is recorded very simply the system will automatically calculate a individual´s risk status.
- Following on from automatic risk calculation there will be Recommended Action for the clinician to follow to ensure the correct pathway of care is followed.
- When the individual´s risk level has been calculated and the recommended action noted the suitable advice leaflet can be provided either from a supply or downloaded directly from the foot screening form
The SCI-Diabetes foot screening tool is not only for recording of information following the screening process it is to ensure that every individual has an assigned risk status, which they understand and know what it means for them, with their risk of developing a foot ulcer which could lead to an amputation automatically calculated. This will also ensure a suitable treatment/management plan can be implemented, according to risk, in a nationally agreed standardised way across Scotland.
The sharing of this information electronically prevents duplication, enables GP contacts to be met and to deliver the Quality strategy outlined in the Diabetes Improvement Plan: Diabetes Care in Scotland: Commitments for 2021 – 2026 [.pdf, 676MB].
04: The procedure (NHS Scotland)
Aim and equipment (1/17)
Aim
The aim of carrying out a foot screening is to identify the presence of risk factors for diabetic foot complications which could lead to ulceration and subsequent amputation such as – Neuropathy, Peripheral Arterial Disease (PAD), Significant structural abnormalities, Significant callus, previous ulceration and the inability to self care. These risk factors should be explained to the individual in a way that they understand them and know what they mean to them.
Equipment
The only piece of equipment that is required to carry out a simple, evidence based, foot screening is a 10g monofilament. The monofilament used should be of good quality such as those manufactured by Bailey Instruments or Owen Mumford and should be used and replaced as per manufacturers instructions to ensure that the monofilament remains accurate. The length of time a monofilament will remain accurate will vary according to it’s frequency of use but Bailey Instruments and Owen Mumford recommend changing the monofilament after approximately 6 months of use. Many clinics use monofilaments much longer than this which can result in less accurate testing.

Neurothesiometer
The Neurothesiometer is a device that tests an individual’s vibration perception threshold (VPT) and monitors diabetic neuropathy by measuring vibration sense. The device graduates in vibration intensity which ranges from 1 – 50 volts.
If a value of <25 volts is entered in the box provided on the SCI-Diabetes form individuals risk will not change but if a value of >25 volts is entered then the individuals risk will change in the same way as if they could not feel 8/10 of the monofilament sites.
Some clinics use the Neurothesiometer as part of the screening process but although it can be used it is not routinely required for screening but can be useful as part of a more ‘in depth’ assessment in specialist centres.






